APPLICATION
A Major Unmet Need in Cardiovascular and Dialysis Care
Hundreds of thousands of coronary bypass surgeries and millions of hemodialysis patients depend on vascular grafts each year. However, small-diameter synthetic grafts (<6 mm) are not approved for these indications due to poor long-term patency.

Coronary Artery Bypass (CABG)
- 850,000+ CABG procedures annually1. Although not widely used, synthetic small-diameter grafts have limited durability with 30–60% patency at 1 year, declining to below 25% by 3–5 years.2
- Up to 30% of patients undergo redo or complex CABG procedures due to the lack of suitable autologous conduits.3
Key insight: A reliable off-the-shelf graft would support the substantial share of CABG patients without adequate autologous vessels.
Limited conduit availability remains a major constraint in CABG. A reliable off-the-shelf graft could expand treatment access, improve procedural efficiency, and unlock significant value in a large cardiovascular market.
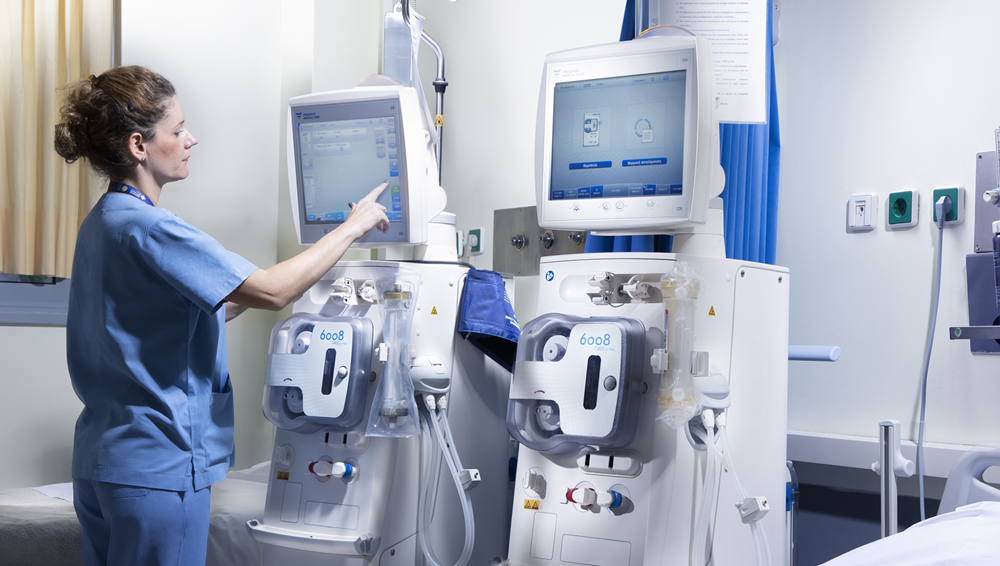
Dialysis Access (AVF / AVG)
- Millions require long-term hemodialysis access.4
- Autologous fistulas (AVF):
20–40% require reintervention within the first year. Early failure often leads to catheter dependence and infection.5 - Prosthetic AV grafts (ePTFE):
40–60% primary patency at 1 year, <25% by 2–3 years.6 More than 50% of patients require at least one reintervention annually. Intervention burden averages 1 to 2+ procedures per patient per year.7
Key insight: Both AVF and AVG suffer from high early failure rates, driving significant clinical workload and repeated interventions.
Frequent access failure and repeated interventions continue to challenge dialysis care. A durable off-the-shelf graft could help reduce intervention burden and support long-term vascular access in a growing dialysis population.
References
- Nalysnyk, L. et al. (2003) ‘Adverse events in coronary artery bypass graft (CABG) trials: a systematic review and analysis’, Heart, 89(7), pp. 767–772. Available at: https://doi.org/10.1136/heart.89.7.767.;
Taggart, D.P. (2022) ‘Coronary artery bypass surgery’, Medicine, 50(7), pp. 445–448. Available at: https://doi.org/10.1016/j.mpmed.2022.04.009. ↩︎ - Pashneh-Tala, S., MacNeil, S. and Claeyssens, F. (2016) ‘The Tissue-Engineered Vascular Graft-Past, Present, and Future’, Tissue Engineering. Part B, Reviews, 22(1), pp. 68–100. Available at: https://doi.org/10.1089/ten.teb.2015.0100.;
Desai, M., Seifalian, A.M. and Hamilton, G. (2011) ‘Role of prosthetic conduits in coronary artery bypass grafting’, European Journal of Cardio-Thoracic Surgery, p. S1010794010010274. Available at: https://doi.org/10.1016/j.ejcts.2010.11.050. ↩︎ - Armstrong, E.J. et al. (2017) ‘Incomplete Revascularization Is Associated With an Increased Risk for Major Adverse Cardiovascular Events Among Patients Undergoing Noncardiac Surgery’, JACC. Cardiovascular interventions, 10(4), pp. 329–338. Available at: https://doi.org/10.1016/j.jcin.2016.11.001.;
Ghandakly, E.C. and Bakaeen, F.G. (2025) ‘Multivessel coronary disease should be treated with coronary artery bypass grafting in all patients who are not (truly) high risk’, JTCVS open, 24, pp. 264–268. Available at: https://doi.org/10.1016/j.xjon.2024.10.014.;
Rufa, M.I. et al. (2024) ‘The impact of incomplete revascularization on survival in minimal invasive off-pump coronary artery surgery: a propensity score analysis of 1,149 cases’, Journal of Thoracic Disease, 16(7), pp. 4504–4514. Available at: https://doi.org/10.21037/jtd-24-387.;
Soukup, C.R. et al. (2021) ‘Rate of Incomplete Revascularization Following Coronary Artery Bypass Grafting at a Single Institution Between 2007 and 2017’, The American Journal of Cardiology, 144, pp. 33–36. Available at: https://doi.org/10.1016/j.amjcard.2020.12.064. ↩︎ - Bello, A.K. et al. (2022) ‘Epidemiology of haemodialysis outcomes’, Nature Reviews. Nephrology, 18(6), pp. 378–395. Available at: https://doi.org/10.1038/s41581-022-00542-7. ↩︎
- Anderson, E.M. et al. (2025) ‘The Impact of Reintervention on Arteriovenous Fistula Maturation and Functional Patency in the Hemodialysis Fistula Maturation Study’, Kidney Medicine, 7(8), p. 101036. Available at: https://doi.org/10.1016/j.xkme.2025.101036.;
Cristino, D. et al. (2025) ‘Patency and maturation rates after forearm arteriovenous fistulas: systematic review with meta-analysis’, Journal of Nephrology, 38(8), pp. 2111–2127. Available at: https://doi.org/10.1007/s40620-025-02346-x. ↩︎ - Halbert, R.J. et al. (2020) ‘Patency of ePTFE Arteriovenous Graft Placements in Hemodialysis Patients: Systematic Literature Review and Meta-Analysis’, Kidney360, 1(12), pp. 1437–1446. Available at: https://doi.org/10.34067/KID.0003502020 ↩︎
- Harms, J.C. et al. (2016) ‘Outcomes of arteriovenous fistulas and grafts with or without intervention before successful use’, Journal of Vascular Surgery, 64(1), pp. 155–162. Available at: https://doi.org/10.1016/j.jvs.2016.02.033. ↩︎